

Study published in The Lancet indicates what the country will need to spend to provide basic cancer screening and care to patients



A report published in the international journal, The Lancet, has drawn attention to poor infrastructure and treatment facilities for cancer patients in India, which is leading to high cancer mortality.
To deliver even a basic cancer screening and treatment package in rural India, 15 states would need to find an additional US $1.6 million a year, (not taking into account inflation), and eight of these states would need an additional US $16 million ever year, the report states.
Roughly one million new cases of cancer are added every year in India, which is one-fourth of that recorded in Europe. However, nearly 70 per cent cancer patients die in India. This ratio indicates that fewer than 30 per cent of Indian patients with cancer survive five years or longer after diagnosis.
By contrast, in North America and western Europe, five-year survival for patients with all types of cancers is about 60 per cent, says the three-part report. The first part of the report gives a macro picture of cancer-related morbidity and mortality in India. The second part focuses on research in India and the third part looks at implications of policies in the country.
The authors conclude that delayed diagnoses and inadequate, incorrect, or sub-optimum treatment are the chief factors for poor cancer survival in India. Nearly 92 per cent patients from rural households first consult private practitioners, 79 per cent of whom are not qualified in allopathic medicine.
Insurance schemes are of little benefit
To improve the situation, investments are to be made in building adequate infrastructure. The authors estimate that 45,000 new health facilities are needed in rural areas. The additional amount to be incurred by the states, as authors propose, will be required for cost-effective population-based packages of clinical care of cancer. According to the authors, private financing is not the solution, since this approach will only drive cost escalation, inequity, and fragmentation.
| Cancer cases and increased spending required |
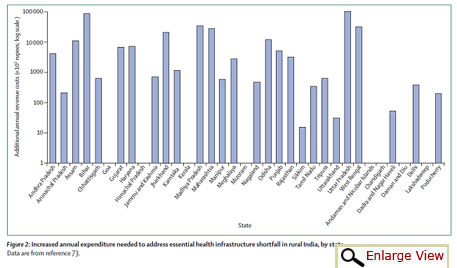 |
Public sector and community-based insurance schemes, too, fail to address the challenges posed by cancer because they focus on inpatient care. There is one Central government-run scheme, Rashtriya Swasthya Bima Yojana, and 17 state-specific schemes (Rajiv Aarogyasri Scheme in Andhra Pradesh and Chief Minister’s Comprehensive Health Insurance Scheme in Tamil Nadu, to name two).
There are some community-run initiatives, too, such as those of Self-Employed Women’s Association, and Action for Community Organisation, Rehabilitation and Development. However, most of these initiatives were not designed to address the complexity and cost of cancer care. RSBY, for example, focuses on inpatient care, and not chronic illnesses like cancer.
However, investment in high-technology, and methods to take treatment to the peripheral part of the country, is missing in the country. Palliative care, childhood cancer, surgery, radiotherapy, health systems and services research, and outcomes research do not attract much attention to study.
The effort of all research and investment in infrastructure should lead to reduction suffering due to cancer. The country looks ill-equipped for the same. The average economic cost of treating a typical cancer patient in a government facility in India has been calculated at about Rs 36,812 (US $593). India’s annual income per person is only US $1,219, and 27.5 per cent of the population lives on or below US $0.4 per day. The advanced nature of most cancers and their effect on household finances make cost-effective screening an important part of delivering affordable cancer care in India.
Stress on early detection, treatment
Some states, like Tamil Nadu, have achieved effective screening coverage. The authors point out that what works in Tamil Nadu will work in other states too and that replication of good practices should begin. One major recommendation of the authors is a cost-effective cancer screening programme across the country. Setting up basic infrastructure will ensure quick detection and better care.
|
Study findings at a glance
|
Report: World Cancer Factsheet
Report: Punjab state report on cancer awareness & symptom based early detection campaign
Report: District Faridkot pilot project report on cancer awareness campaign
Feature: Pattern and trends of cancer in Odisha, India
We are a voice to you; you have been a support to us. Together we build journalism that is independent, credible and fearless. You can further help us by making a donation. This will mean a lot for our ability to bring you news, perspectives and analysis from the ground so that we can make change together.

Comments are moderated and will be published only after the site moderator’s approval. Please use a genuine email ID and provide your name. Selected comments may also be used in the ‘Letters’ section of the Down To Earth print edition.