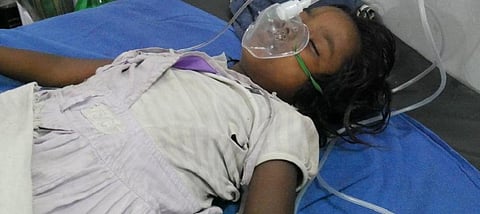

When seven-year-old Khushi Yadav started running a high temperature, her family first took her to a community health centre (CHC), five kilometres from their home in Padrauna, the district headquarter of Kushinagar in northeastern Uttar Pradesh. The temperature didn't drop after the medication prescrived there and she was next taken to the district hospital, some 25 km away. She remained admitted there a week before eventually being transferred to Baba Raghav Das (BRD) Medical College, some 65 km away, in neighbouring Gorakhpur.
Nothing uncommon for BRD, which was in national news over a series of deaths of babies and children two years ago. A lack of awareness about and trust on primary healthcare centres (PHC) lead patients and their families to travel long distances to avail medical help. While they lose crucial time for early treatment, tertiary care hospitals get swamped. In the case of BRD and Gorakhpur, add another crucial factor to that: acute encephalitis syndrome (AES).
A PHC should be more than enough to handle cases of AES; yet patients are taken directly to big hospitals or private doctors. AES cases haven't yet come up this season in UP — though the situation in neighbouring Bihar is worrisome — but it might. BRD, meanwhile, is crammed already with patients, some of whom have travelled 100 km.
The only tertiary care centre in eastern UP has only 428 beds dedicated for AES — that's what is supposed to cater to patients from Gorakhpur as well as a host of nearby districts, including Kushinagar, Sant Kabir Nagar, Azamgarh, Deoria and Maharajganj, apart from Bihar and even Nepal. The hospital’s Ward No.100, which houses the Paediatric Intensive Care Unit (PICU) and High Dependent Unit (HDU), is synonymous with encephalitis. It is the ward where more than 30 children died in 48 hours due to lack of oxygen cylinders in August 2017.
Better or worse
Infrastructure has improved since then. Also, PHCs have been strengthened to reduce the load on BRD. mini-PICUs were set up at eight CHCs in the region, each with three beds and ventilators for encephalitis patients. About 20 CHCs in Gorakhpur have been converted into encephalitis treatment centres (ETC). The government also set up an ambulance service.
“(AES) cases will start with the monsoon underway. Paramedics and paediatricians have been trained to deal with encephalitis patients; necessary medicines and equipment have been stocked,” said Suresh Kumar Dudi, one of the two paediatricians at a CHC mini-PICU in Piprauli block.
What remain challenges are to raise awareness in the community and gain people’s trust so that approach PHCs and the CHC, instead of directly visiting big hospitals or private doctors and quacks, Dudi said.
Sirjavati, a resident of Belghat block, some 55 km from BRD Medical College, took her nine-year-old daughter Isha to a private practitioner nearby, even though the nearest PHC-cum-CHC, which now functions as an ETC (Encephalitis Treatment Centre), was just four km away.
Her fever subsided after medication and injections, but rose again next day. She was again taken to the same doctor twice. After her condition worsened, Isha was admitted to the CHC with seizures, which then referred her to District hospital and from there to BRD Medical College, where she died on May 15, 2019.
“I didn’t think she would be provided treatment there. We thought it is just fever and she will be okay,” Sirjavati said, when asked why she did not take Isha to the nearest CHC first.
“This is the problem. Parents keep medicating wrong and bring children here only when the condition is out of our hands,” said a staff nurse posted at the CHC, which has seven AES cases on record till now.
This not only increases the load at BRD but the children also lose out on the initial diagnosis, crucial for the treatment, the doctors pointed out.
However, patients also complain of lack of proper facilities and doctors at these CHCs.
These fears are not always misplaced, DTE found.
Incomplete centres
Of the 19 CHCs converted into ETCs, none had paediatricians or any facility for tests or sampling.
“There should at least be a facility for CSF (cerebrospinal Fluid) count to which is critical to establish the diagnosis. People think when they will anyway be referred later, so why not they go themselves,” said a staff at an ETC in Harnhi of Khajni block.
Almost all ETCs have staff shortage. At the Harnhi CHC, there are only two doctors (one MBBS and another Ayush) against the post of six.
“There are fewer encephalitis cases right now but even those who have, they are taken directly to BRD. People also know there is no paediatrician here or no blood sampling facility,” said Dr AP Maurya.
There is a shortage of specialised staff at CHCs, SK Tiwari, chief medical officer at Gorakhpur, told DTE.
“We don’t have that many in the pool. The human resource is complete in mini PICUs, but CHCs are a problem. Overall there is a vacancy of 26 paediatricians,” Tiwari said.
He, however, added that the trend of going directly to BRD has reduced in the last two years, which could be attributed to campaigns like ‘Dastak’ — launched by the UP government to eradicate AES and JE disease.
But, there still remains a long way for the eradication of encephalitis and it demands a national programme on the lines of polio or tuberculosis eradication, said RN Singh, a private paediatrician, who was earlier with BRD.
“We could eradicate polio completely because there were sustained efforts. Even till date polio vaccinations are given. Why can’t we do the same for encephalitis, which affects hundreds of children every year in Bihar, UP, Assam, West Bengal, etc” Singh said.
In fact, a national programme for prevention and control of encephalitis was finalised in 2014 by the then Congress government but never launched after a change in power at the Centre.
“The programme was made in 2012 by Group of Ministers and even Rs 4,000 crore was said to be allocated to it. But it never took off. If countries like Taiwan, South Korea, and China can eradicate encephalitis, why can’t we? There is a lack of political will to launch that programme which is lying with red tape,” Singh said.